Virus in the Dust: Exposing the Fabricated Contagion of Andes Hantavirus
Why the "human-to-human" panic ignores the simple reality of common environmental exposure to rodents on the ship
By Peter A. McCullough, MD, MPH
As an epidemiologist, I know contact tracing studies are inherently flawed. So I was immediately suspicious of the claim that Hantavirus Andes strain had jumped from zoonotic to human-to-human spread. This claim is very likely to be false and should not be the basis for the global public health response to the Hantavirus outbreak from rodents on board the MV Hondius.
🔬 Scientific Evaluation: Reassessing Transmission Pathways of the Andes Orthohantavirus
1. Introduction
The Andes orthohantavirus (ANDV) is uniquely recognized within the Hantaviridae family for its putative human-to-human transmission. While this claim has become a foundational pillar in epidemiological modeling and public health policy, the scientific evidence base remains largely speculative. This report critically examines the methodological limitations inherent in existing contact tracing studies and argues that the assertion of direct human-to-human transmission lacks the rigorous validation required by controlled, empirical investigation.
2. The Confounding Variable: Environmental Exposure
The primary challenge in attributing ANDV infection to human-to-human contact lies in the ubiquity of the virus’s primary reservoir, the long-tailed pygmy rice rat (Oligoryzomys longicaudatus).
🏚️ The “Common Environment” Hypothesis
Existing epidemiological studies frequently rely on retrospective contact tracing to establish transmission chains. However, these investigations often fail to adequately isolate participants from shared environmental risks.
Aerosolized Particulates: ANDV, like other hantaviruses, is primarily shed in the urine, feces, and saliva of infected rodents. These excretions dry into dust, which can remain infectious for extended periods in enclosed spaces.
Inadequate Site Assessment: In many documented “human-to-human” cases, the transmission occurred within households or rural dwellings. These environments are frequently contaminated with rodent excreta. Current contact tracing methodologies often assume that if no rodent was seen, no rodent exposure occurred. This assumption ignores the reality that microscopic viral particles in house dust are sufficient for inhalation or mucosal contact.
A rigorous scientific framework must rule out the possibility that both the “index” case and the “secondary” case were independent victims of the same contaminated environmental reservoir before concluding that direct transmission took place. In the absence of comprehensive environmental sampling—specifically, testing dust and surfaces for viral RNA at the time of exposure—the environmental transmission hypothesis cannot be dismissed.
4/1/26 Ship departs likely with infected rodents on board
4/11/26 Dutch man dies on ship
4/24/26 Spouse of Dutch man disembarks in St Helena with his body and dies shortly afterwards
4/24/26 Ill British man disembarks and airlifted to Johannesburg improved now out of ICU
4/24/26 n=28 passengers get off and remain well except Swiss man
4/24/26 Swiss man with mild symptoms has Hantavirus found and genotyped (below)
5/2/26 German dies on ship in harbor at Cape Verde (authorities refused to let the ship dock at the port because of the suspected hantavirus outbreak)
5/2/26 WHO locks passengers in cabins with infected rodents/ventilation system, fresh air on deck not permitted
5/10/26 Remaining passengers disembark in Canary Islands
5/10/26 Ill French woman flown from Tenerife to a France ICU (first victim from WHO lockdown)
5/11/26 MV Hondius, still virus-contaminated, likely with rodent reservoir sets sail with 30 crew and medical personnel to Rotterdam, Netherlands
3. The Absence of Empirical Validation
The standard for establishing a novel transmission pathway is high. To definitively conclude that a virus has transitioned from zoonotic to human-to-human spread, one must move beyond correlational field data. Toledo et al evaluated the published studies and concluded that person-to-person spread had not been demonstrated.
🚫 Lack of Challenge Studies
Currently, there exists a complete absence of isolated human challenge studies. While ethical constraints are understood, the lack of clinical validation leaves a significant interpretive gap.
Biologic Plausibility vs. Proof: While viral shedding in human bodily fluids has been documented, the viability and infectiousness of the virus via human-to-human routes remain unproven.
The Zoonotic Baseline: The Hantavirus genus is characterized by its strict association with rodent hosts. For a virus to jump from a zoonotic cycle to sustained or even sporadic human-to-human transmission, distinct evolutionary adaptations are typically required—none have been found in the current strain. The current literature has yet to provide a robust, mechanistic explanation of how ANDV bypasses the natural species barrier so effectively in human populations without intermediate animal hosts.
4. Methodological Critiques of Current Surveillance
The widespread acceptance of human-to-human ANDV transmission relies heavily on the strength of contact tracing data. Yet, these studies suffer from significant selection bias:
Recall Bias: Participants in high-stress, post-outbreak scenarios are naturally prone to recall interactions with other people, while often overlooking mundane environmental exposures like sweeping a floor or entering an unventilated storage room.
Lack of Genomic Precision: While viral sequencing has shown links between cases, it does not distinguish between a direct human-to-human transmission chain and a shared, localized environmental source that mutated or persisted in a specific rodent population.
5. Conclusion
The assertion that Andes orthohantavirus has definitively transitioned to human-to-human transmission is premature and conceptually fragile. When environmental contamination—a well-established risk factor for all hantaviruses—is not meticulously excluded, the “transmission” observed in clusters may simply be a reflection of communal exposure to a shared, contaminated micro-environment. Until controlled studies are performed and environmental variables are rigorously accounted for, the scientific community should maintain a skeptical perspective on the viability of human-to-human spread and should not participate in global fear-mongering over a hantavirus contagion.
Please subscribe to FOCAL POINTS as a paying ($5 monthly) or founder member so we can continue to bring you the truth. Alter AI may be used to assist in searches, synthesis, and review.
Peter A. McCullough, MD, MPH
President, McCullough Foundation
FOCAL POINTS has partnered with Patriot Mobile to defend your medical freedom. Join Patriot Mobile today!
📚 References
Martinez, V. P., et al. (2005). “Human-to-human transmission of Andes virus.” Emerging Infectious Diseases. (Critique: Focuses on descriptive epidemiology; lacks environmental viral load analysis).
Padula, P. J. (2011). “Epidemiology and ecology of hantavirus infections in South America.” Virus Research. (Context: Emphasizes the primary role of Oligoryzomys species in viral maintenance).
Schmaljohn, C., & Hjelle, B. (1997). “Hantaviruses: A global disease problem.” Emerging Infectious Diseases. (Foundational context on the environmental stability of hantaviruses in rodent dust).
Tigabu, A., et al. (2020). “Environmental risk factors for hantavirus infection: An updated review.” Frontiers in Microbiology. (Critique: Highlights the persistent under-reporting of environmental contamination in indoor settings).
Joao Toledo, Michelle M Haby, Ludovic Reveiz, Leopoldo Sosa Leon, Rodrigo Angerami, Sylvain Aldighieri, Evidence for Human-to-Human Transmission of Hantavirus: A Systematic Review, The Journal of Infectious Diseases, Volume 226, Issue 8, 15 October 2022, Pages 1362–1371, https://doi.org/10.1093/infdis/jiab461



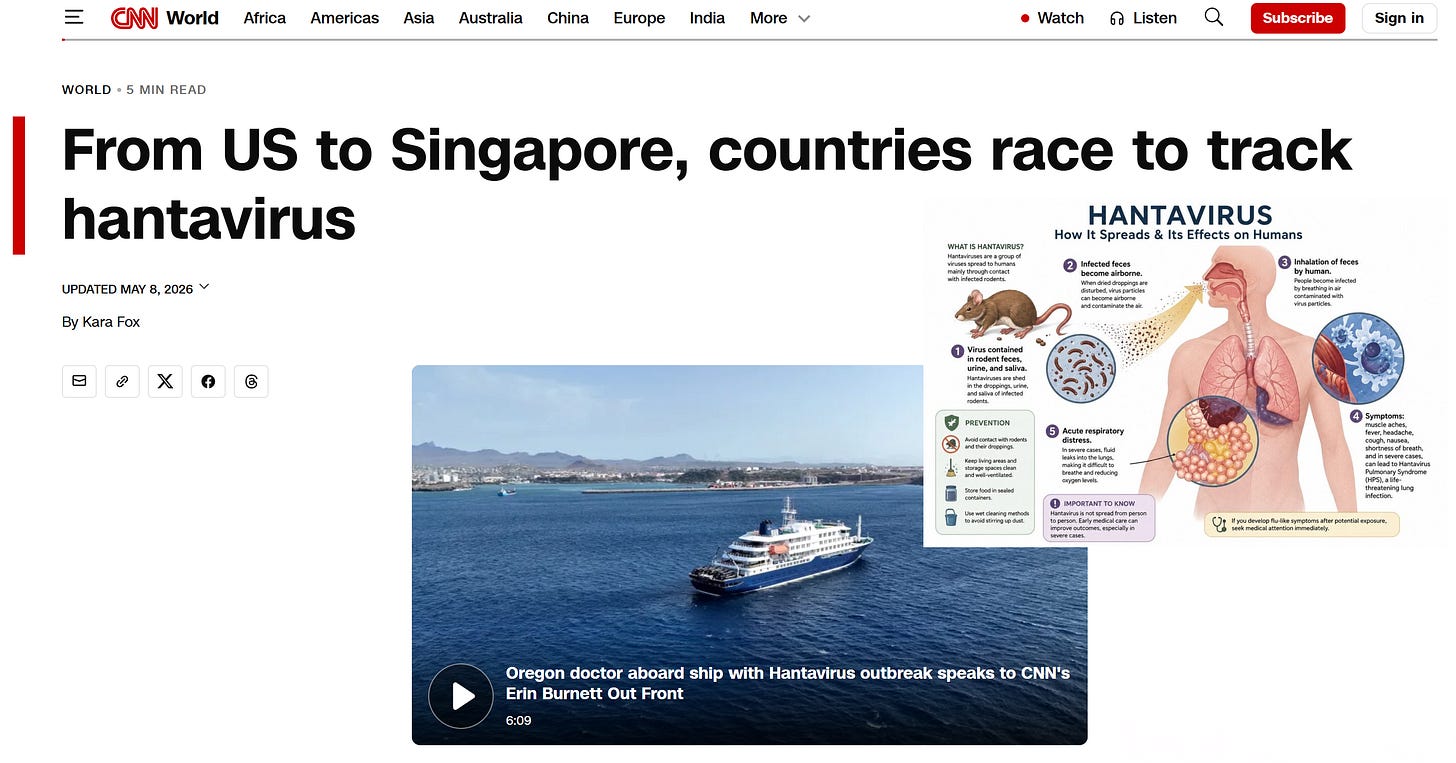


Another example of how hard it has become to trust our public health agencies
Should the last sentence have a not: “should not participate”?